Pleural Effusion
Fluid around the lung: understanding why it happens and how surgery helps.
What is the Pleural Space?
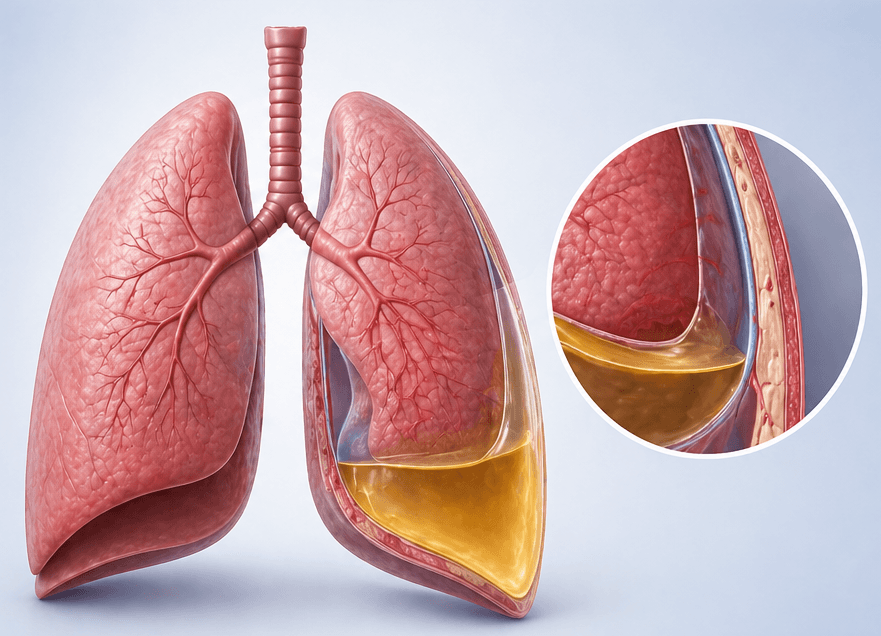
Causes of Pleural Effusion
Pleural effusions can generally be categorized as either transudates, which are precipitated by systemic dysfunctions that change the fluid pressure or protein balance, or exudates, which are precipitated by local inflammation, infection, or malignancy. It is often caused by heart failure, liver cirrhosis, nephrotic syndrome (transudates), pneumonia (parapneumonic effusion), tuberculosis, malignancy, and pulmonary embolism, and autoimmune diseases such as rheumatoid arthritis and lupus (exudates).
Special attention should be paid to malignant pleural effusion. It happens when the cancerous cells implant in the pleura, which is usually due to lung cancer, breast cancer, mesothelioma, lymphoma, and ovarian cancer, and affects fluid reabsorption. Malignant effusion is usually huge, recurrent, and progressive and severely compromises the quality of life.
Empyema: When the Effusion Becomes Infected
The effusion of fluid (around pneumonia) may develop into empyema- raw pus in the pleura. Empyema needs to be drained urgently. In case of untreated hemodialysis, fibrin septa develop, and loculations develop that do not easily drain. A completely formed empyema (fibrothorax) encloses the lung, and to re-expand it, it must be decorticated (surgically removed) to remove the thick fibrous rind.
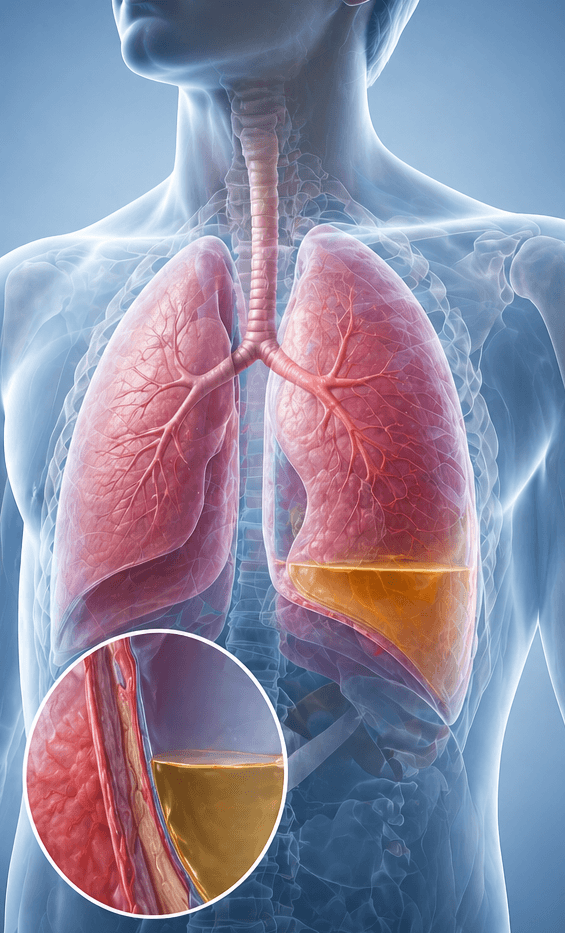
Symptoms
Diagnosis
Treatment Options
ThoracocentesisAspirin of the fluid using a needle with the help of ultrasound. Diagnostic and symptomatic. No established treatment of recurrent or malignant effusions. |
Intercostal Drain (ICD)A tube through pleural space to drain constantly. Applied to empyema, massive effusions and serves as the initial intervention before the definitive treatment. |
VATS DecorticationMinimal invasive surgery to excise fibrous peel which encloses the lung in organised empyema. Enhances complete lung re-expansion and infection resolution. |
PleurodesisTo prevent the recurrence of malignant effusion, chemical ablation of the pleural space (with talc or other agents) is used. Can either be thoracoscopically (VATS) or through drain. |
Indwelling Pleural CatheterPlural catheter An indwelling pleural catheter (IPC) can be used to permit recurring household drainage in patients who are incapable of surgery or in whom the pleura are trapped by the lung (e.g., trapped lung). This will go a long way in enhancing the quality of life and lower the hospitalization of the advanced cancer patients. |
Surgical Decortication for Fibrothorax
Struggling with Recurrent or Complex Pleural Effusion?
Book Appointment
+91-9920024001
9920024001
