Thymoma & Myasthenia Gravis
Surgical removal of the thymus gland, transforming outcomes in chest tumours and autoimmune disease
The Thymus Gland
Thymoma: The Anterior Mediastinal Tumour
Thymoma is the most common tumour of the anterior mediastinum in adults, typically presenting in the fourth to sixth decade of life. It arises from thymic epithelial cells and is classified by the WHO into types A, AB, B1, B2, B3, and thymic carcinoma, with increasing grades corresponding to more aggressive behaviour, greater invasiveness, and higher recurrence risk.
Approximately 30–40% of thymoma patients also have myasthenia gravis. Other paraneoplastic syndromes associated with thymoma include pure red cell aplasia, hypogammaglobulinaemia, and various autoimmune disorders.
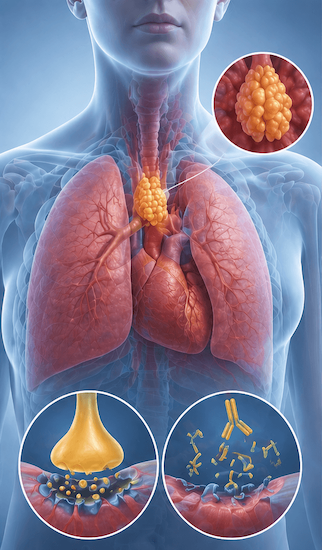
Symptoms of Thymoma
Many thymomas are discovered incidentally on chest imaging done for other reasons. When symptomatic, patients present with chest pain or tightness, breathlessness (if the tumour is large), cough, superior vena cava (SVC) syndrome (facial swelling, neck vein distension, headache due to venous compression), or features of an associated paraneoplastic syndrome. Locally invasive thymomas may erode into the pericardium, pleura, or great vessels.
Myasthenia Gravis
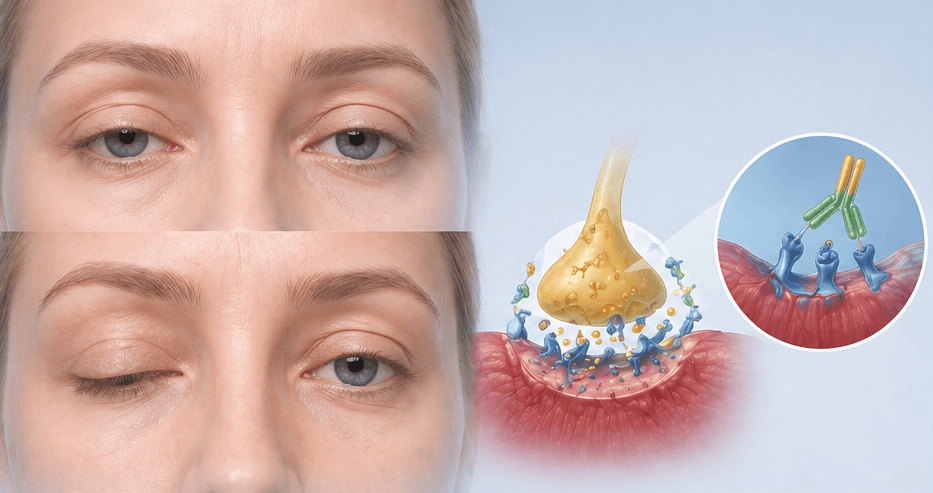
Myasthenia gravis (MG) is an autoimmune disease in which antibodies (most commonly against acetylcholine receptors) attack the neuromuscular junction, the connection point between nerves and muscles. The result is fatigable muscle weakness that worsens with activity and improves with rest. MG typically affects the ocular muscles first (causing drooping eyelids, ptosis, and double vision, diplopia), followed by the bulbar muscles (causing swallowing and speech difficulties) and eventually limb and respiratory muscles.
Respiratory crisis, myasthenic crisis, is a life-threatening emergency in which respiratory muscles fail, requiring mechanical ventilatory support. Management involves immunosuppression (pyridostigmine, steroids, azathioprine), plasma exchange or intravenous immunoglobulin for acute crises, and, crucially, thymectomy.
Why Thymectomy for Myasthenia Gravis?
Surgical Treatment: Thymectomy
Historically, thymectomy required median sternotomy (splitting the breastbone). Minimally invasive approaches have largely replaced this, including VATS thymectomy (via small chest wall incisions), robotic thymectomy, and transcervical approaches, offering equivalent or superior completeness of resection with dramatically less surgical trauma, shorter hospital stays, and faster return to normal life.
Staging of Thymoma (Masaoka)Stage I: Completely encapsulated. Stage II: Microscopic/macroscopic capsular invasion. Stage III: Invasion of adjacent organs. Stage IV: Pleural/pericardial spread or distant metastasis. Surgery alone may be curative for stages I–II. |
Adjuvant TreatmentPost-operative radiotherapy is considered for stages II and III thymoma. Chemotherapy is used for unresectable or metastatic disease.
Stage IV pleural disease may still benefit from selected surgical resection combined with systemic therapy. |
Thymoma or Myasthenia Gravis Diagnosis?
Book Appointment
+91-9920024001
9920024001
