Aspergilloma, Bronchiectasis & Hydatid Cyst
Chronic lung conditions where timely surgery prevents life-threatening complications
Three distinct but important chronic lung conditions, aspergilloma (a fungal ball in a lung cavity), bronchiectasis (permanent airway dilatation and damage), and pulmonary hydatid cyst (a parasitic cyst of the lung), share a common thread: they each carry risks of major haemoptysis and progressive lung destruction, and each may require surgical intervention when medical management is inadequate.
Aspergilloma
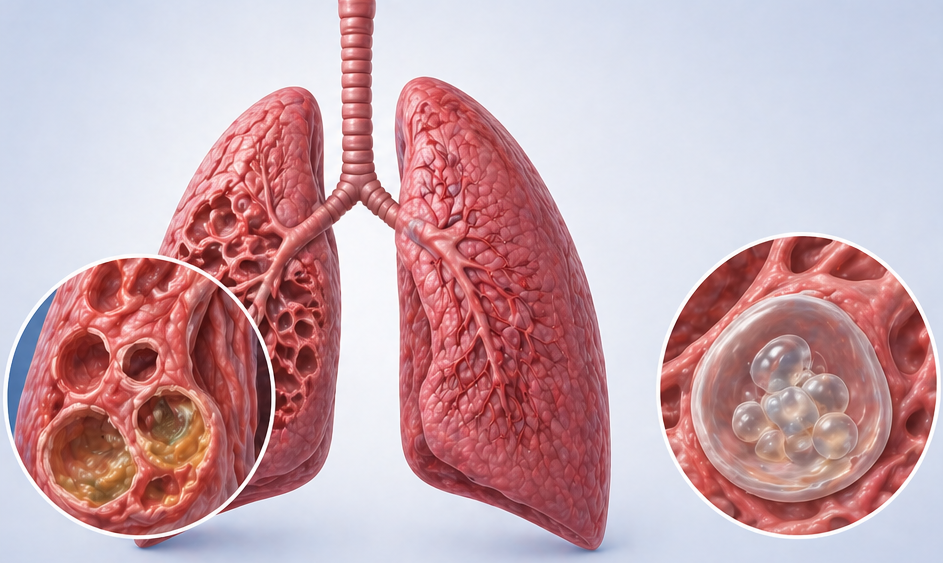
The condition is classified as simple aspergilloma (a single cavity with a relatively intact surrounding lung) or complex aspergilloma (multiple cavities, thick cavity walls, significant underlying lung disease, and bilateral involvement). Complex aspergilloma carries a far worse prognosis and poses a greater surgical risk.
Symptoms of Aspergilloma
Many aspergillomas are asymptomatic for prolonged periods, discovered incidentally on imaging. The most feared complication is haemoptysis, coughing up blood, which occurs in up to 75% of patients and can be massive and life-threatening. The mechanism involves invasion of bronchial blood vessels within the cavity wall by fungal hyphae or by an inflammatory reaction around the cavity. Other symptoms include chronic cough, weight loss, and fatigue. Fever and worsening breathlessness suggest secondary bacterial infection or progression to invasive aspergillosis.
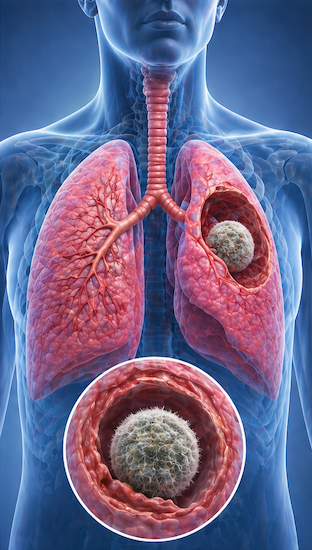
Surgery vs. Embolization for Aspergilloma Haemoptysis
Bronchial artery embolization (BAE) can temporarily control haemoptysis by blocking feeding vessels, but recurrence rates are high (40–60% within one year) because the underlying aspergilloma and cavity persist. Surgical resection, removing the affected lobe or segment, offers a definitive cure with low recurrence of haemoptysis. For fit patients with localised disease and adequate lung reserve, surgical resection is the preferred approach.
Surgical Treatment of Aspergilloma
Surgery for aspergilloma ranges from wedge resection or segmentectomy for small peripheral lesions to lobectomy for larger or centrally located disease. The operation requires meticulous technique to prevent spillage of the fungal ball (which can seed the pleural space, causing pleural aspergillosis). Cavernostomy, surgical opening and cleaning of the cavity without formal resection, is an option for high-risk patients with inadequate lung reserve who cannot tolerate lobectomy. Post-operative antifungal therapy (voriconazole) is continued to prevent recurrence.
Bronchiectasis
Patients suffer from a daily productive cough with large volumes of purulent sputum, recurrent chest infections, haemoptysis (which can be massive), breathlessness, and fatigue. Bronchiectasis has a significant impact on quality of life and, when widespread, leads to progressive respiratory failure.
When Does Bronchiectasis Need Surgery?
VATS lobectomy or segmentectomy for localised bronchiectasis provides excellent results with low morbidity. For bilateral or diffuse disease, surgery is not curative but may be palliative (e.g., resecting the most diseased segment responsible for repeated haemoptysis). Lung transplantation is the ultimate option for end-stage bilateral bronchiectasis in young patients, particularly those with cystic fibrosis.
Pulmonary Hydatid Cyst
The hydatid cyst has three layers: the outer pericyst (host tissue reaction), the middle laminated membrane (the parasite’s outer layer), and the inner germinal layer (which produces brood capsules, scolices, and daughter cysts). Pulmonary hydatid cysts can grow to enormous sizes, 10–15 cm, and produce pressure effects on the surrounding lung.
Symptoms and Diagnosis
Surgical Treatment of Pulmonary Hydatid
For smaller peripheral cysts, the approach involves careful enucleation of the intact cyst (cystotomy technique). For larger, ruptured, or complicated cysts, lobectomy may be necessary. The VATS approach is increasingly used for accessible cysts in experienced hands. Medical therapy with albendazole is used pre-operatively to reduce cyst viability, prevent recurrence, and treat spillage. Long-term follow-up is necessary because recurrence can occur even years after apparently successful surgery.
Albendazole in Hydatid Disease
Prevention of Hydatid
Aspergilloma, Bronchiectasis, or Hydatid Cyst?
Book Appointment
+91-9920024001
9920024001
